Address:
20 Park Plaza, Suite 804
Boston, MA 02116
978-888-7999
Address:
20 Park Plaza, Suite 804
Boston, MA 02116
978-888-7999

By Dr. James Katz, MD, MPH
Inflammation of the gums is associated with heart disease, stroke, diabetes, rheumatoid arthritis, and pneumonia. DNA from oral bacteria have been found in damaged heart valves and lumbar discs. Biannual professional cleaning reduces the risk of pneumonia in the elderly by 80%. Oral inflammation can be present as gingivitis (affecting the gums) or periodontitis (affecting the roots of the teeth). It elevates inflammation throughout the body and damages the circulatory system in the same fashion that elevated cholesterol, blood sugar, or blood pressure does. Reducing this inflammation will improve one’s overall health. Here is a program for better tooth brushing. It will improve your teeth, breath, and reduce cavities.
The bacteria that cause oral inflammation live primarily at the base of the teeth under the edge of the gums. These pockets are their reservoir: under conditions of proper nutrition and maintenance, and in the absence of chronic illness, they are relatively non-toxic. In the diagram below (from The American Academy of Periodontology), these bacteria would be found on both the “Healthy” and the “Periodontal Disease” sides in the pink areas. On the “healthy” side, the gums are adherent to the tooth surface. On the “periodontal disease” side, the gums have receded creating pockets in which enormous amounts of bacteria grow. The results include bad breath, cavities, gingivitis, and even erosion of the jaw bone and loss of teeth.
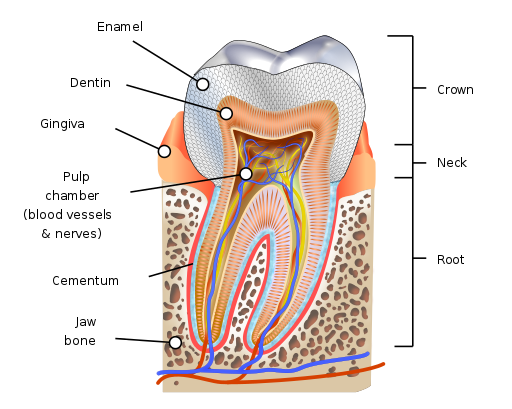
When exposed to sugars and carbohydrates, the oral bacteria undergo explosive growth and spread over all the surfaces of the teeth. They produce corrosives that dissolve enamel and create microcavities. When the bacteria have exhausted their nutrient supply, those on the teeth die and form deposits (plaque), but others remain in the pockets at the base of each tooth. The microcavities, if repeatedly exposed to corrosive bacteria, evolve from soft spots to holes in the enamel which must be fixed. However, exposed to the proper mix of food, saliva, and minerals (including calcium and fluoride), microcavities can heal without drilling and filling.
The lower the sugar/carb content of your diet, the better. More rapidly dissolving carbohydrates will accelerate more bacterial growth. The worst foods are sticky candies, which provide prolonged bacterial stimulation while they dissolve, and frequently right on the gum line. Even worse, the action of chewing can push the candy further into pockets. We have deep emotional attachments to different foods. They can be consumed if we understand how to minimize their effects. (See sections below on Saliva, Brushing, and Flossing)
There are beneficial substances one can consume including green tea, aloe vera, xylitol, folic acid, and pomegranate. They are weak anti-bacterials, and the oral bacteria repopulate quickly. These ingested products cannot penetrate the pockets. They are helpful, but not curative.
We produce approximately one trillion bacteria per day in the mouth. Share on XWe produce approximately one trillion bacteria per day in the mouth. The microbiome is the approximately 400 trillion bacteria inhabit our gut. They make crucial products, such as blood clotting factors, without which we would die. They make neurotransmitters, which are absorbed from the gut, cross into the brain, and are used by our nervous system. These bacteria do not lead isolated lives; they are actually part of elaborate signaling networks, and it starts in the mouth. You produce approximately 1 trillion bacteria a day in the mouth. Your goal in oral health is to improve the balance of good bacteria, while understanding that wiping out any bacteria perceived as bad may actually disturb the network, causing greater harm than good.
Consuming water dilutes the bacterial load, especially if you can swish it around your mouth. Share on XAvoid alcohol containing mouthwashes. In their place, gargle with water, salt water, or water with a small amount of bicarbonate. For the most part, an electric toothbrush, with a pressure sensor to prevent over brushing, does the best balance of removing plaque without damaging teeth. Brush every surface of your mouth including the gutters at the top and bottom of your cheeks, as well as brushing your tongue. Some people advocate tongue scrapers. Use as little toothpaste as possible; some studies show a dry toothbrush removes more plaque than a wet one or one with toothpaste. Floss every time you brush and floss at every meal. Make sure to see your dentist for teeth cleaning. There are oral probiotics, however, there no long-term studies available. Saliva flow is beneficial for your teeth and gums – sugarless gum is a great agent for this. When nothing else is available, just swirling water around your mouth spitting it out is beneficial.
Saliva has several properties that benefit oral health. As a liquid it reduces the concentration of food molecules in the mouth as well washing them downstream. Saliva contains proteins that bind bacteria. It also digests some sugars. Saliva is rich in calcium and phosphate, which are the building materials for reversing processes of cavity formation.
At any one time, you have about twenty areas on the 164 tooth surfaces that are softening and leeching Share on XAt any one time, you have about twenty areas on the 164 tooth surfaces that are softening and leeching calcium as they are attacked by the acids from the oral bacteria. Unremitting acid presence (continuous consumption of sugary sweets) will eventually wear a hole in the tooth (now it’s a cavity) and you win a trip to your dentist. But if the tooth is exposed to a healthy flow of calcium, phosphate, and fluoride, the micro cavity will heal and the enamel will re-harden. Good sources of calcium are milks, yogurts, and cheeses. Phosphates are found in natural grains and cereals (NOT the cereals in the grocery store – they have too much added sugar!) High fluoride mouthwashes are available. They are vital to this process.
Anything that increases the flow of saliva improves oral health. Celery sticks, toothpicks, and sugarless gum all work well. The sooner one utilizes one of these agents after eating, the better. That includes after snacks as well as after meals. It is true that sugarless gum produces microscopic amounts of unpleasant substances, but at concentrations that make them irrelevant (except for rare genetic conditions) to health.
Consuming water dilutes the bacterial load, especially if you can swish it around your mouth before swallowing. Drinking water during, and after meals, as well as after snacks, will help.
Overly vigorous tooth brushing is part of the cause of a vicious cycle that results in gum recession and periodontal disease. Most people brush their teeth with too much pressure. Trying to get a toothbrush bristle into the 2-3mm space below the gum line without damaging the gums is very difficult. What most people consider normal brushing will damage the gums. Once damaged, the microscopic pockets in the gums become better incubators for the periodontal bacteria, which inflame the tissue, making it more susceptible to damage.
An alternative is to get an electric toothbrush (Oral-B, Phillips Sonicare are the best-known brands). The brush takes care of the strokes; you mind the pressure. Run the brush under hot water prior to use to soften the bristles. Rely on the vibratory mechanism to move the brush thousands of times per minute. Let the toothbrush do the cleaning – you concentrate on pressing very lightly.
There are bacteria on all the surfaces in your mouth – cheeks, roof, and tongue as well as teeth Share on XThere is no one best pressure for tooth brushing for everyone – but there is a best pressure for each individual. The more extensive the inflammation in one’s mouth, the more gently one should brush. Harsher cleaning will worsen periodontal inflammation.
Your dentist/dental hygienist can help you learn how much pressure to use. Have them stand behind you while both of you face a mirror and have them literally hold your hand and demonstrate the right technique. Repeat the drill at your next few cleanings to get it down. Some toothbrushes have flexible necks to protect from excess pressure, but in tests the flexible necks don’t work.
There are bacteria on all the surfaces in your mouth – cheeks, roof, and tongue as well gums and teeth. A gentle pass with the electric toothbrush will do wonders to dislodge these surface-dwelling bacteria. You would do well to swish some mouthwash/water to get the bacteria before they resettle. Be careful to avoid the base of the tongue. The “gag” reflex resides at the base of the tongue. The sensitivity of the “gag” reflex changes from day-to-day, so even if it feels comfortable the first time you try this, a surprise is always possible.
A dental irrigator (Water Pik) is the tool for cleaning out the 2-3mm pockets at the base of each tooth. It will also remove food from between teeth and dental work. Irrigating with water is good; using salt or bicarbonate may work better. Large concentrations of hydrogen peroxide is harmful. If you are traveling, ToiletteTree makes a USB rechargeable irrigator that collapses for packing. However, leave the little gate “open” so it can dry between uses.
A full set of teeth contain over 160 surfaces that need cleaning. Flossing cleans tooth surfaces between teeth and some of the pockets. Floss comes in rolls, but this type of floss requires the user to place their fingers in their mouths. It makes flossing a two-handed operation. If you have large fingers and a small mouth, it is difficult.

Interdental flossers (single use pieces of plastic that hold a three/quarter inch piece of floss or small brush) are extremely useful, in addition to or in place of regular floss. They are less bulky to carry and can be used and discarded through the day. They can be used with one hand. One doesn’t have to put fingers in one’s mouth. Several hints on use: hold the flosser vertically to get between the anterior teeth, tip it almost horizontal to reach the back teeth. While the end of the flosser might be pointed, it is too hard to be used to dislodge food from between teeth.
The process of cavity formation is dynamic. The plaque bacteria release enzymes and acids that cause a rough spot in the tooth enamel. This rough spot is not sensitive, so the earliest part of cavity formation is silent. You can reverse a cavity when it is at the microscopic stage. By shifting your diet to be richer in calcium and avoiding acidic foods, you can reduce the number of dental interventions. You should not enrich your diet with calcium pills because there is significant evidence that high pulses of calcium can deposit in artery walls, while gradually absorb calcium from foods does not. As for the acidic foods you enjoy, continue to have them, but try to come up with foods to balance them. For example, if oranges are a favorite, cut them up and combine them with the yogurt of your choice. Similarly, cheese, nuts, salmon, sardines, beans, and green leafy vegetables (think spinach) are great sources of calcium. If these are part of the mix of foods on the plate, they balance each other out.
American Academy of Periodontology. “Healthy Smile May Promote A Healthy Heart.” ScienceDaily 9 January 2008. 20 August 2008 Markers of systemic bacterial exposure in periodontal disease and cardiovascular disease risk”
Biesbrock et al. Assessment of Treatment Responses to Dental Flossing in Twins. Journal of Periodontology, 2006; 77 (8): 1386 DOI: 10.1902/jop.2006.050399
Mealey BL, Rose LF. Diabetes mellitus and inflammatory periodontal diseases. Curr Opin Endocrinol Diabetes Obes. 2008 Apr;15(2):135-41.
Moutsopoulos NM, Madianos PN. Low-grade inflammation in chronic infectious diseases: paradigm of periodontal infections. Ann NY Acad Sci. 2006 Nov;1088:251-64.
de Pablo P, Dietrich T, McAlindon TE. Association of periodontal disease and tooth loss with rheumatoid arthritis in the US population. J Rheumatol. 2008 Jan;35(1):70-6.
Demmer RT, Desvarieux M. Periodontal infections and cardiovascular disease: the heart of the matter. J Am Dent Assoc. 2006 Oct;137(Suppl 1)4S-20S.
Abou-Raya S, Abou-Raya A, Naim A, Abuelkheir H. Rheumatoid arthritis, periodontal disease and coronary artery disease. Clin Rheumatol. 2008 Apr;27(4):421-7.
Niemiec BA. Periodontal disease. Top Companion Anim Med. 2008 May;23(2):72-80.
Meyer MS, Joshipura K, Giovannucci E, Michaud DS. A review of the relationship between tooth loss, periodontal disease, and cancer. Cancer Causes Control. 2008 May 14