Address:
20 Park Plaza, Suite 804
Boston, MA 02116
978-888-7999
Address:
20 Park Plaza, Suite 804
Boston, MA 02116
978-888-7999

What I prescribe for insomnia patients, and I use myself
You fall asleep with ease, then wake at three in the morning. Your mind races — tomorrow’s presentation, today’s argument, a vague sense you’ve forgotten something important. You are not ill. You are not in pain. You are simply, maddeningly, awake.
I know this state well. As a physician, I have spent years counseling patients on sleep hygiene while quietly ignoring my own bad habits. Medical training is excellent preparation for disregarding insomnia and its complications.
Being wide awake at 3 AM is early morning awakening (EMA). It is common. Our society is at war with sleep. Electric lighting, cellphone and computer screens, alarm clocks, and stress reduce rest.
One in three Americans reports insomnia. Early morning awakening — the habit of rising hours before the alarm and failing to return to sleep — is the most frequent pattern.
Poor sleep harms the body. Chronic early waking is associated with elevated cortisol, impaired glucose control, weakened immunity, greater cardiovascular risk, cognitive decline, and a higher incidence of depression. Studies link it as well to Type 2 diabetes and Alzheimer’s disease.
But insomnia doesn’t end when the night does. EMA type sleep loss causes a thirty percent higher risk of motor-vehicle accidents. Impaired judgement and attention, slow reaction time, and fatigue, and “microsleeps,” all contribute to automobile crashes. And some crashes are fatal.
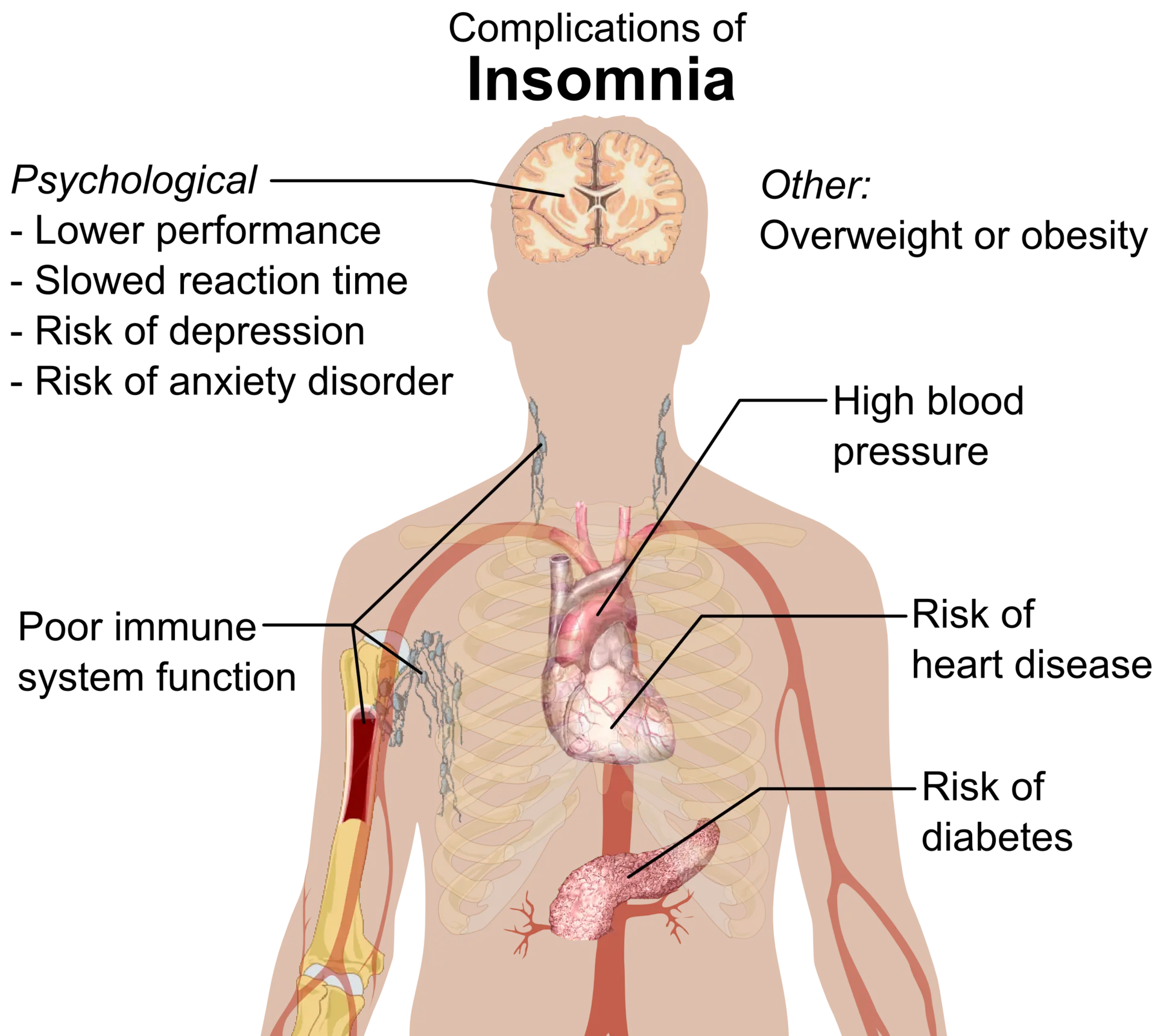
Image Credit GgGevorg Wikicommons
The more you dread waking early, the more likely you are to do so. Anxiety feeds on itself. Many with early morning awakening fall asleep easily, only to be pulled back to consciousness by a stray thought in the dark, stranded and alert.
I counsel patients in sleep hygiene: regular bedtimes; a dark, quiet, cool room; daytime exercise; no alcohol or caffeine in the evening. When this fails, I may prescribe sedatives such as benzodiazepines or zolpidem. These drugs can cause dependence, grogginess, and cognitive side effects. Withdrawal often brings rebound insomnia, worse than before, and the patient reaches for another pill. In my practice, alternate-night dosing or very low doses limit habituation.
Melatonin dominates the over-the-counter market. It is often misused. My patients’ typical dose is 5 milligrams at bedtime — too much, too late, and bought in bulk from a warehouse store because the bottle said, “sleep support.” The drug at that dose lingers into morning, causing fatigue and poor concentration. The American Academy of Sleep Medicine does not recommend melatonin for insomnia. Melatonin is better reserved for circadian rhythm disorders such as jet lag or shift work, at about 0.5 milligrams taken two to three hours before bedtime.
The current gold standard for insomnia is Cognitive Behavioral Therapy for Insomnia, or CBT-I. It combines behavioral changes with psychological techniques and has remission rates between 50 and 70 percent. It works, but it requires six to eight sessions with a trained therapist, and getting an appointment may take months.
Cognitive shuffling was developed by Dr. Luc Beaudoin, a cognitive scientist, AI expert, and adjunct professor at Simon Fraser University. The idea is deceptively simple.
“Sleep onset isn’t instantaneous. It proceeds gradually,” Beaudoin explains. “It’s a unique time in the day when you’re thinking isn’t really connected.”
How it works: choose simple, neutral, unrelated objects. Example: apple, mailbox, canoe, yellow raincoat, lighthouse. No drama. No meaning. No plot. Visualize one object for 3–10 seconds. Then drop it. Pick another. Do not connect them. A canoe may not float. A mailbox does not receive mail. This is not a Pixar short.
If your mind starts scheming, worrying, or composing tomorrow’s email, switch objects. The objects always win. Some people need more structure to the exercise. Pick a letter. Think of objects that start with it. Example: B — balloon, barn, bicycle, blueberry, bridge. Then change letters. This provides order without meaning. Order without meaning is the point.
Continue until sleep happens. For many people, this takes only a few minutes.
Rumination keeps the cortex engaged. A meaningful thought — a worry, a problem — activates the brain’s problem-solving circuits and blocks sleep. Random images prevent narrative. The mind is occupied but not aroused.
The key is randomness. No story. No logic. No connection between images.
“We’re not just distracting the mind,” says Beaudoin. “We’re giving it something to do that mimics how the brain naturally drifts toward sleep.” Dr. Scott Walker, who introduced the technique to millions via TikTok, describes it as “a way to rearrange or reorganize your thoughts, similar to shuffling a deck of cards.”
In a 2016 study, participants using cognitive shuffling reported getting back to sleep easily, less difficulty getting back sleep when EMA occurred and better sleep quality. Further research is underway. No cognitive technique, including this one, should stand alone.
Cognitive shuffling works best as part of a bigger strategy. Here’s what the science supports.
Move in the morning. Any outdoor morning exercise reduces nighttime awakening, though purists will insist on thirty minutes of moderate aerobic exercise. Just keep aerobics away from bedtime. Vigorous exercise within two to three hours of sleep can raise your core temperature and delay sleep onset.
Cut caffeine earlier than you think. Caffeine has a half-life of five hours. That 3 p.m. coffee is still 50 percent active at 8 p.m. Sleep specialists recommend cutting it off by 1 p.m. if you’re prone to waking early. I learned this the hard way after years of a 4 p.m. “just one more cup” habit that I had heroically convinced myself wasn’t the problem.
“If someone drinks a lot of coffee before bed, they shouldn’t expect cognitive techniques to help them fall asleep,” Beaudoin said plainly.
Stop drinking alcohol. I tell patients to stop using alcohol. They smile the smile of someone who has no intention of doing that. Then I mention that alcohol converts into acetaldehyde, a known carcinogen, which increases the risk of breast, colorectal, esophageal, liver, and head and neck cancers. The smile fades. I’ve had many patients reduce their intake and a few stop entirely.
Dim the lights. Bright screens and overhead lights suppress natural melatonin secretion and throw off your circadian rhythm.
Write your worries down. A brief journaling session in the early evening — getting your concerns out of your head and onto paper — reduces the mental backlog that tends to surface at 3 a.m.

Picture composed by Google Nano Banana
Catch the sunrise. The eastern sky becomes rosy, pink starting twenty minutes before official sunrise. The invisible near-ultraviolet and near-infrared light at that time resets your circadian rhythm as nature designed. Walk outside for the sunrise light. By the time the sky is blue, the special near frequencies are gone.
But if you still wake in the middle of the night, reach for cognitive shuffling. Start visualizing images. Keep them random, unrelated, and emotionally neutral. Don’t weave them into stories.
The goal isn’t perfect sleep. The goal is to give your brain a way out of the spiral.
“It’s simple, imaginative, and easy to understand,” says Beaudoin. “That is why it has resonated.”